Announcement
Keeping patients safe at home with virtual wards
Dec 1, 2022

Virtual wards are helping hospitals and clinicians reimagine their approach to healthcare. The National Health Service (NHS) aims to provide an extra 2,500 virtual ward beds to increase capacity and operational resilience this winter, an important step in providing a solution to many of the patient safety challenges facing the NHS today.
In a recent webinar, Dr. Harpreet Sood, Vice President of Primary Care and Partnerships at Huma; Dr. Arrash Yassaee, Global Clinical Director of Evidence Generation and Information Governance at Huma; Prof. Mike Bewick, former National Deputy Medical Director at NHS England; and Mandie Welch, Advanced Nurse Practitioner at Cwm Taf Morgannwg University Health Board (CTM UHB), discussed the challenges, opportunities and improvements to patient safety they are seeing today with digital health wards. Here, we share some of their insights on how digital wards have changed the way they deliver patient care.
Increasing patient safety with patient-focused design
Too often, patient safety is a reactive process, when in reality it should be thought of proactively. By seeking out opportunities to improve patient care and safety, we can improve our healthcare system. Huma’s patient-centred approach to digital health is helping to bring this technology to the forefront and increase patient safety. In order to get this technology into patients’ hands, the design needs to be user-friendly and simple.
“When setting up a virtual ward, getting patients involved from the development stage to get their views on what they want out of an app is vital to the success of the program and platform,” said Mandie Welch, who helped launch an ongoing pilot with our remote monitoring technology to care for her heart failure patients at CTM UHB.
By learning what patients and clinicians want from an app, we can ensure digital health is not just more noise in the system. Based on the patient feedback we have received so far, Huma has been able to implement important new features such as two-way conversations and video links to better connect patients with providers.
Digital health has an important role to play in reducing patient harm and improving safety. The evidence around the value of using virtual wards is increasing, and digital health is helping to reinvent what healthcare looks like, putting patients and their safety at the forefront.
Virtual wards enable patients who need in-person care to get faster access
Many hospitals and inpatient clinics struggle to find space for patients – an issue that is potentially contributing to as many as 500 excess deaths a week2. By using validated and evidence-based digital technologies, we can reduce this unnecessary harm. Through virtual wards, clinicians can improve patient monitoring, allowing them to bring in patients sooner if needed, but also keeping them at home for as long as possible.
The lack of inpatient space also has consequences for those in need of an elective procedure – the current waiting time is 52 weeks or more3. The very real patients behind this statistic are often facing deteriorating medical conditions with long-term consequences if they do not receive treatment when they need it. Remote patient monitoring allows healthcare providers to review the patients on that list to identify and triage those who need to be seen sooner.
Another risk of the current system is “the longer you stay in hospital, the more likely you are to get iatrogenic disease,” according to Prof. Mike Bewick. “Releasing people earlier through a digitally-enabled tool helps reduce that risk.”
With virtual wards, providers are able to see patients faster and capture the relevant clinical data via our web-based platform. Our hospital partners are already able to discharge patients sooner with the data provided by virtual wards. One physician partner shared, “Because we were able to keep an eye on their heart rates and blood pressure on a daily basis, this facilitated them going home earlier. It also encouraged medication compliance.” The virtual ward platform empowers patients to take control of their health, giving them real-time monitoring and allowing them to feel better, faster.
Patients have shared that Huma’s virtual ward platform “helped me know that somebody was looking after me.” Another shared that they appreciate not having to worry about making long drives to the clinic, taking time off work, or finding someone to bring them to an appointment.But what about those patients who do not have access to a smartphone or cannot use the platform due to technology barriers? By using virtual wards, hospitals and clinics are able to free up more space for frail and underserved patients, increasing their access to healthcare and allowing them to be seen sooner. Virtual ward technology could help reduce occupied beds, freeing up space for those with greater need.
Longitudinal data from digital health improves medication management
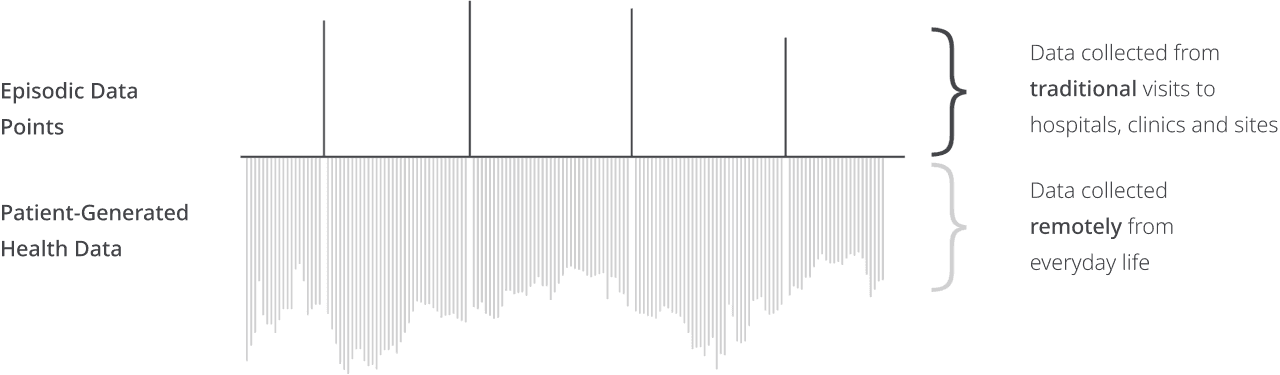
Digitalization has revolutionized the approach to virtual wards and gives providers an opportunity to look at patients in different environments. When a patient comes in for an in-office visit, the physician must base their treatment plan on that single snapshot of how the patient is at that moment. Meaning they miss out on clinically relevant day-to-day information. With virtual wards, providers can view longitudinal data to help them prescribe the best medications for what patients are really experiencing. Oftentimes, blood pressure medications may be unnecessarily prescribed when a patient presents with high blood pressure from “white coat syndrome” at an in-office appointment. With a longitudinal view, providers can review data to see what a patient’s health is like when they are relaxed at home, allowing them to not only prescribe more effectively but also monitor and intervene quicker.
This new approach has the potential to increase patients’ quality of life, reduce discomfort, and lead to better disease management. Before digital health was available, medication optimization could take 6-9 months. Now, providers can quickly review data and make changes weekly, in some cases patients can be medically optimized 76% faster.
Virtual wards optimize patient care and care delivery
Throughout the pandemic, digital technologies were crucial to maintaining and evolving care. Now, these approaches must be embedded into the everyday delivery of care. Setting up a digital ward can seem challenging as change is often slow in the healthcare space.
“The single most important thing is working with partners who understand the process of putting the convenience of the patient first and foremost,” said Dr. Arrash Yassaee. “Essentially, digital can't be forced on people. It needs to be a choice, so it needs to be done in a way that is as appealing to all parties as possible. And if we do that, the potential could be limitless.”
By getting clinical teams involved from the start and choosing user-focused platforms, we can help better manage chronic and acute diseases. The future of health is digital, and Huma’s digital, single platform-based solution is underpinned by a growing amount of evidence.
Welch concluded, “I can't go back to the way I was working before because it's a real disservice to my patients when they're not optimized as quickly as they are being now. We've already seen a reduction in our accident and emergency through the app users and a reduction in the time spent in a coronary care unit bed.” Huma’s partners have seen significant efficiency savings and a corresponding reduction in healthcare costs, alongside the wider impacts that better patient outcomes can bring to productivity.